Thyroid Conditions
Dr Ben Lancashire is a specialist endocrine surgeon. He has expert training in surgical management of thyroid gland disorders.
What is the thyroid gland?
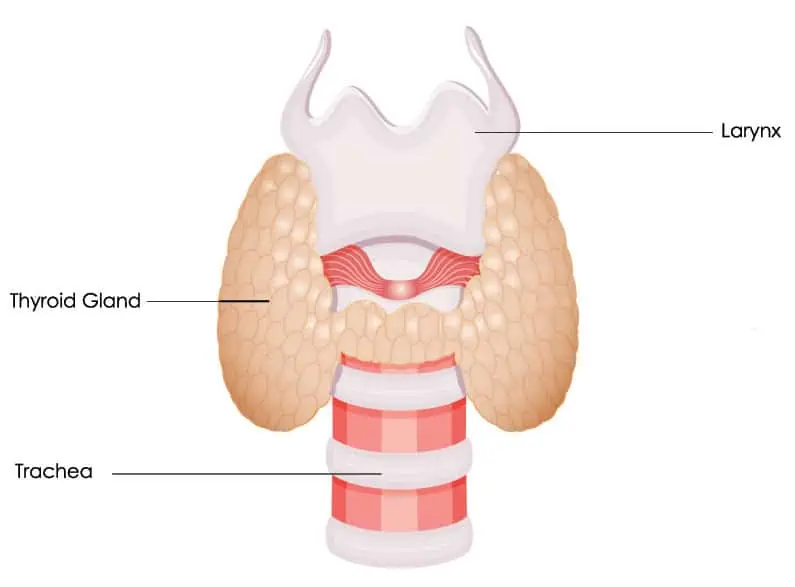
The thyroid gland is a butterfly-shaped gland in the front of the neck. It sits in front of the windpipe (trachea), just below the voice box (larynx).
The thyroid produces a hormone called thyroxine (or T4). The active form of this hormone plays an important role in growth, development, and regulating your body’s metabolism. This can affect your weight, temperature, heart rate, energy levels and mental alertness. Your GP will be able to arrange tests to see if your thyroid gland is overactive or underactive.
Thyroid nodules
Thyroid nodules are lumps that develop in the thyroid gland. Thyroid nodules are extremely common, and incidence increases with age. About 50% of people will have at least one thyroid nodule by the age of 50 (and 90% of us by age 80). They can range in size from a few millimetres to a several centimetres.
The key questions we seek to answer regarding thyroid nodules are:
- Is it cancerous?
- Is it causing symptoms by pressing on other structures in the neck, like the trachea (windpipe) or oesophagus (food pipe)?
- Is it producing too much thyroid hormone?
Evaluation of thyroid nodules usually includes blood tests, an ultrasound, and a biopsy (Fine Needle Aspiration or FNA). The biopsy is usually done by a radiologist under the guidance of an ultrasound, with local anaesthetic. Sometimes other scans are arranged to help determine the size and activity of the nodule.
Because the thyroid has such a rich blood supply and is surrounded by many very important other structures (like the trachea, blood vessels and nerves), a relatively small sample is taken. This means that the pathologist looking at the sample may not always be able to give a definitive result. A complex international scoring system (called the Bethesda System) is used to guide doctors and patients about the risk of the nodule being cancerous.
Dr Lancashire will be able to explain what your biopsy result means and consider it together with your blood tests and scan results to help determine the best management plan, and whether surgery is the right option for you.
Thyroid Cancer
Thyroid nodules are very common – but less than 1% of all of those are cancerous. There are four main types of thyroid cancer:
- Papillary thyroid cancer (80%)
- Follicular/Hürthle thyroid cancer (14%)
- Medullary thyroid cancer (4%)
- Anaplastic thyroid cancer (2%)
The prognosis for the most common types of thyroid cancer (papillary and follicular) is generally excellent. Medullary thyroid cancer is often associated with genetic endocrine disorders, and it tends to spread earlier than papillary cancers. Anaplastic thyroid cancer is extremely rare and carries a very poor prognosis despite surgery.
Many thyroid cancers are treated with a total thyroidectomy (complete removal of the thyroid gland). Some thyroid cancers require additional neck lymph node surgery and/or treatment with radioiodine.
Graves’ Disease
Graves’ Disease is an autoimmune disease which causes the thyroid gland to produce too much thyroid hormone. There is often a genetic component to the condition (meaning that there are often other relatives with the condition) and it is much more common in women.
Most people diagnosed with Graves’ disease see an endocrinologist before they see a surgeon. Medications or radioactive iodine (RAI) may be recommended and work very well. If the treatments do not work, the side effects are not being tolerated, or the thyroid gland is very big (called a goitre), you may be referred to a surgeon with a recommendation to have your thyroid removed.
Hashimoto’s Thyroiditis
Hashimoto’s thyroiditis is the most common disorder of the thyroid. It is also a type of autoimmune disorder where immune cells attack the thyroid, causing inflammation. This condition effects the thyroid in different ways – sometimes the gland can become very enlarged (goitre), but often, the inflammation damages the gland in a way that makes it underactive. This leads to a condition called hypothyroidism.
Specific treatment is not usually required for Hashimoto’s thyroiditis, but like any thyroid gland, it can also develop nodules that need to be evaluated.
Dr Lancashire works in consultation with the Brisbane Thyroid Cancer Clinic at the Royal Brisbane & Women’s Hospital. He will discuss what type of surgery he recommends with you, and any other potential treatments you may require.


